Amputations in Malvinas
Eduardo
C. Gerding
Amputation is a
surgical act that causes an ireversible change in the person
subjected to it. 14 The amputation of a limb
is a dilemma to which a doctor is submitted to under certain critical
situations. Unsuccessful attempts to save an unrecoverable limb are associated
with high morbidity and often result lethal to the patient.39
Military personnel are at grave
risk for landmine and shrapnel injuries, amputation (occurring in 10%–16% of
wounded soldiers) Roughly 3500 traumatic amputations are performed each year on
soldiers, despite multiple preventive programs instituted by the military and
other agencies.( Starnes BW, Beekley AC,
and Sebesta JH. et al. Extremity vascular injuries on the battlefield:
tips for surgeons deploying to war. J Trauma. 2006 60:432–442.)
In England and Wales there are more than 80,000 people who have
lost one or more members: 27,000 due to wars and 60,000 due to injuries or
illnesses. Approximately 3,500 new cases are sent to the 21 national prosthetic
centers each year. 28
War injuries have caused many disabled men, making
Cambodia the country with the largest number of amputees per capita in the
world. 28
This article
delineates, in relatively simple terms, the experience in amputations among Argentine
and British military during the Malvinas
conflict.
Without further
digging into technical details, which are the responsibility of the orthopedic
surgeon, this paper tries to contribute to a better knowledge for both the
Argentine Association of Wounded in Malvinas and for the Subdirectorate of War
Veterans through the Prosthesis Area of the Special Benefits Department
of the National Institute of Social Services for Retirees and Pensioners
(INSSJP).
Historical background 2,41
There are references
of Neolithic amputations of fingers which have been dated to about 5000 B.C. Amputations
of hands were sometimes done as a mean of verifying numbers of prisoners taken
in battle. 41
Artificial
hands made of iron were used by knights in the 15th .An
example of this is the Alt-Ruppin iron hand
found in 1863 in the River Rhine and that, endowed with a rigid thumb,
allowed to flex the remaining fingers, in pairs, on the palm.28
Evidence of foot
amputations performed in Peru in 300 BC has also been found. 41
Perhaps the first use
of a limb prosthesis is that of a Persian soldier, Hegesistratus, who was
reported by Herodotus to have escaped about 484 B.C. from stocks by cutting off one of
his feet and replacing it with a wooden one. 2 . The oldest known artificial limb in existence was a
copper-and-wood leg unearthed at Capri, Italy, in 1858, which was supposedly
made about 300 B.C. 2,41
Verduin (1696) devised the first prosthesis with
free knee joint. In 1800 James Pott, began the construction of wooden
prosthesis, against the general opinion of manufacturing them in iron, as their
weight prevented any effective function. Pott added to his wooden prosthesis,
knee joints in steel and an articulated foot provided with tendons that
provided a dorsal elevation when flexing the knee (this prosthesis was used and
disclosed by the Marquis of Anglesey, and is known as the "Anglesey leg").28
Hippocrates described
the use of ligatures, but this technique was lost during the Middle Ages. It
was reintroduced in 1529 by Ambroise Paré, a French military surgeon. As a
result, amputations were increasingly used as a salvage measure since the
survival rate was much higher when ligatures were used. 2
In 1674, William
Richard Morel introduced the tourniquet, which gave another impetus to amputation
surgery. Paré carried out the first
procedure of disarticulation of the elbow in 1536. Sir James Syme described in
1843 a procedure for the amputation of the ankle.
The introduction of
the antiseptic technique in 1867 by Lord Lister, a student and son-in-law of
Syme, contributed greatly to the overall success of amputation surgery, as did
the use of chloroform and ether at almost the same time.2
In 1898 Dr. Robert
Rieder of the University of Bonn went to Istanbul to reform Turkish medical
education and, while there, fell down fracturing his hip and leg. The treasurer
of II. Abdűlhamit broke his leg and suffered 3 amputations.
For this reason four army officers were sent
to Paris to study prosthetics. The Turkish naval officer Hűseyin Rifat returned
from Europe and established the first prosthetic workshop called Tersane-i
Alati Nazikiye.
During the First
World War, Ottoman Empire´s naval
officer Kazim Elgűn was sent to Vienna for 4 years to learn prosthetics and on
his return he worked with Professor Dr. Besim Őmer Akaim. 4
The concept of
kinematics to push upper extremity prostheses directly by muscle contraction
was introduced by Giuliano Vanghetti in 1898. This last attempt thus to improve
the function of the Italian soldiers to whom the Abyssinians amputated their
hands. Vanghetti's partner, Antonio Ceci, performed the first such operation on
humans in 1900.
In Germany,
Ferdinand Sauerbruch (1916) developed the skin-lined muscle tunnel. In
Argentina, in the 1920s. Guillermo Bosch Arana carried out clinical studies of
this procedure .2
In Great Britain, the
Limb Fitting Centre at Queen Mary's
Hospital, Roehampton, expanded its research effort shortly after the end of
World War II and became known as the Biomechanical
Research and Development Unit. 2
AMPUTATIONS
Indications 5
Indications 5
1. Extremities with
severe compromise of skin, muscle, bones and irreparable nerve injuries.
2. Severe local
infection which, despite adequate surgical measures and antibiotic treatment,
endangers life.
3. Death of the limb,
vascular gangrene when the vascular repair fails or is impracticable.
4. Massive septic
gangrene. Cellulitis or anaerobic myositis confined to a single muscle group
can be treated with resection and hyperbaric chamber.
Objectives of the Primary Amputation 5
1. Resect all dead, contaminated and
blunt tissue.
2. Allow primary deferred closing
3. Leave a stump acceptable for later
equipment
Note: Method of urgency. This amputation, also called ¨in sausage¨, has its precise indications in
emergency surgery; it is proposed, above all things, to save the patient´s . It
is performed when a severe trauma has destroyed part of a limb and presents a
large, bloody surface that has been in contact with septic bodies; it is also
indicated in cases of severe septic processes, particularly due to anaerobes.
Primary Deferred Closure 5
The experience of the
Service of Traumatology of the Malvinas Military Hospital in 1982 confirms the
validity of the concept of primary deferred closure in serious limbs wounds ,
open fractures and stumps. 6
Characteristics of a good stump 28
The most suitable
length of a stump is that which best preserves comfort, function and
aesthetics. The ideal length for amputations below the knee is 12 cm and never
more than 15 cm.
All surgically good
stumps must meet the following three conditions:
Softly conical shape.
Normal sensitivity.
Scar properly located and mobile.
Morbidity and mortality among civilians 36
In Argentina, 48% of amputations are due to diabetes.13
The greatest frequency of amputations due to trauma is found in the decade from 41 to 50 years; due to illness, between 61 and 70 and, due to tumors, between 11 and 20 years.28
Of the 146 patients with traumatic lower limb amputations attended at the Trauma Center of the University of Maryland (USA) 9% died during admission and 3.5% died after being discharged. 67% of the patients were men and 75% were white. 60% of the amputations were in patients under 40 years of age. The most frequent location of amputations is in the lower extremities (10: 3 in relation to the upper extremity).
A study conducted in the Surgical Department of the Municipal Hospital
of Arhus (Denmark) on 109 amputee patients revealed that two thirds of them
could walk with a prosthesis but only half of them could do it with full
capacity. The ability to walk and not suffer pain was better in the
infrapatellar than in the suprapatellar amputees. (Acta orthop. scand. 45. 97-104,1974)
Cause
of disability due to amputations
Studies reveal that the most frequent causes of
disability after a traumatic amputation of lower limbs are: 1) Psychological
illness, 2) Decrease in physical and vocational functionality, 3) Increase in
cardiovascular morbidity and mortality. 29,33,35
The
psychological damage 17
Traumatic amputations
are often linked with intense fear, horror, images of others being injured, and
startling sounds that resurface during rehabilitation (even in the absence of
full criteria for PTSD). ( Parkes CM.. Psychosocial transitions:
comparison between reactions to loss of a limb and loss of a spouse. Br J
Psychiatry. 1975;127:204–210. ) (Bhuvaneswar, Chaya et
al-Reactions to Amputation: Recognition and Treatment-Prim Care Companion J
Clin Psychiatry 2007;9(4):303-308)
A review in India of men with lower
limb amputations due to traumatic causes revealed a prevalence of psychiatric
disorders in 32% to 84%, including depression (10.4 to 63%), PST (3.3 to 56.3).
%) and Phantom Limb phenomenon (14 to 92%) .40
Prostheses only become a substantial
help in the treatment of these psychic alterations when they manage to adapt to
the body schema in a dynamic sense. 28
IRegarding this, Argentine war veterans
have the support of the Islas Malvinas
Armed Forces ´Health Center
Complications
of BKA amputations
The possible complications of BKA are due to: 1) Anesthesia, 2) Infections,
3) Vascular and nervous lesions, and 4) Bleeding and blood clots.
Possible
post-amputation disorders 37
1. Continuous nervous pain
2. Phantom limb
3. Bone spur (heterotopic ossification)
Note: A study conducted at the University of
Maryland Trauma Center on 146 amputees revealed that a quarter of them had
disorders with the residual limb including Phantom Limb Syndrome.36
Phantom
Limb 32
A phantom limb is the sensation that an amputated or missing limb still attached. Despite a great deal of
research on the underlying neural mechanisms of phantom limb pain there is
still no clear consensus as to its cause.
Note: According to Bosman et al, the protective
factors of the Phantom Limb are: 1) Being a male, 2) Amputation of the lower
limb and 3) Interval of time since the amputation.3
Experience of the Argentine Military Health Service 7
Ceballos et al
published a review of 439 medical records of surgical patients injured during the Malvinas war
. It was necessary to perform 40 amputations and half of them where at the toes
level.
Surgical pathology of limbs caused by
combat actions-Cases admitted at the Military Puerto Argentino
(April 12nd to June 15th, 1982). Data represents 22% of the 1990 patients
admitted to the hospital in the same period.
No %
No %
Combat injries:
Sharpnel 183 41.7
Bullets 76 17,3
Explosions 7 1,6
Combat related conditions
Trench foot 173 39.4
Total
439 100,0
Note: It is suspected that some of the bullet wounds were self
inflicted
Shrapnel injury
https://www.google.com.ar/search?q=shrapnel+picture&tbm=isch&source=iu&ictx=1&fir=U3UqNN_1ckLV9M%253A%252C5af8X43GkMYF-M%252C_&usg=__eT8h9LKAwcLORRL26BFPwrGM3gc%3D&sa=X&ved=2ahUKEwjHieet-cLcAhWDgpAKHUTfCMsQ9QEwAnoECAYQCA#imgrc=VdBoFY-TIuWRsM:
Location of wounds by projectiles and
anti-personnel explosives admitted at the Military Hospital of Puerto Argentino.
Those wounded in the limbs represent 73.7% of 361 cases of casualties war
admitted in the same period.
No %
Limbs 266 73.7
Thorax
23 6,4
Abdomen
13 3,6
Head and neck 8 2,2
Multiple wounds and others 51 14,1
Total
361 100,0
Wounded by weapons of war admitted at
the Military Hospital of Puerto Argentino, discriminated by agent.
No %
Sharpnel
256 70,9
Bullets
83 23
Blast 15 4,2
Mine
5 1,4
Granade
2 0.5
Total
361 100.0
Note: 90% of gun shot injuries were in the limbs and 48% in hands and
feet.
Open fractures fractures caused by war weapons admitted at
the Military Hospital of Puerto Argentino. Injuries by anti-personnel explosives
(foot of mine and hand granade) are not included
Shrapnel Bullet Total
No %
Femur
3 - 3 4.6
Shin bone 4 2 6 9.1
Fibula
1 1 2 3.0
Foot bones 2 21 23 34.8
Humerus
7 - 7 10.6
Radius and ulna 1 2 3 4.6
Radius 2 - 2 3.0
Hand bones 1 19 20 20.3
Total
21 45
66 100.0
(Kindly submitted by War Veteran Silvia Barrera)
British Army war veteran Col (Ret)
James Michael Ryan and on his left the Argentine Sergeant War Veteran
Juan Gualberto Vallejos, a native of Corrientes who belonged to the Company A of Regiment 3 who lost his right leg
at Wireless Ridge towards the end of the war. He fought 67 days. As he says "I
was 25 years old when the conflict happened, and thanks to my family I read the gospel and the
message that God had for me. This
last allowed me to overcome the
psychic, social and emotional problems, set aside the resentment and preach the Word of the Lord.
" The veteran is pastor of an evangelical church and since
2006 provides material and spiritual assistance at the Heroes Generation
Foundation. (El Litoral.com.ar)
Amputations per trench foot made at the
Puerto Belgrano Naval Hospital 24
11 patients were
amputated. In all cases, emergency were performed, leaving the stump open.
The amputees were
treated in the hyperbaric chamber in the pre- and post-operative stages. In all
cases the amputation was indicated by suppuration of the lesions.
The level of
amputation was as follows:
Middle
third of leg 2
Upper
ankle joint
2
Tarsus metatarsal
8
Metatarsal-phalanx 2
Partial
amputation of fingers both feet 3
Big
toe 1
Note:
Antibiotic
therapy: Antibiotic treatment was performed in 30 patients. 52% of the cases.
In mild injuries (stage 1) antibiotics were not administered. In severe
injuries (stage 5) antibiotic therapy was performed according to the
antibiogram
Experience of the British Military
Health Service 19,26
Amputations in the British Armed Forces in Malvinas
Two years after the
end of the Malvinas conflict, the British had 38 amputations (32 major and 6
minor amputations), of which 23 corresponded to the Army.
At least 51 British
soldiers have suffered amputations due to injuries suffered in Afghanistan, surpassing
the Malvinas figures.21
Note: Captain Harry Parker, son of Lieutenant General Sir Nick Parker,
the third officer in seniority of the British Army lost his leg by a bomb while
patrolling in Afghanistan and, although the doctors struggled two weeks to save
his limb ,they were unsuccesful.
Indications
Complete
traumatic amputation 13
Gross disruption 7
Primary vascular damage 2
Secondary vascular insufficiency 1
Note: A typical example is the case of
Parachutist Eric Baker (71) years of Doncaster, South Yorkshire who suffered a
fracture in the Malvinas between the 4th and 5th finger. The fracture became infected.
He was admitted and his leg had a BKA. He had to be re-admitted for gangrene
and a new cut 7.5 cm above the knee was
made.31
Distribution of Amputation
Above knee 7(2)
Through knee 1
BKA 11 (7)
Above elbow 2
Below elbow 2(2)
----------------------------------------------------------------
Total
23(11)
Note: The figures in parentheses are cases that occurred after the cease-fire. 48%
(11) of the amputations occurred after the cease-fire. Amputations of fingers
secondary to burns are not included. If we exclude the 11 cases, the amputation
index was approximately 2.5%. None of the patients who arrived at primary
surgical care died. There were no cases of amputations as a result of clostridia.
Land mines
https://www.google.com.ar/search?q=minas+terrestres+argentinas&tbm=isch&tbo=u&source=univ&sa=X&ved=2ahUKEwiE55Ow-MLcAhUFC5AKHWB6C08Q7Al6BAgGEA0&biw=1280&bih=686#imgrc=uw0w-sGh5Lev4M:
Wounding
agent
Anti
personnel mine 9(5)
Mortar/Artillery 3
Gun shot 3
Bomb
2
Sidewinder -(4)
Booby trap -(1)
High Explosives -(1)
Note: United Nations personnel suffered 174
incidents with antipersonnel mines, anti-tank mines and booby traps in
Yugoslavia between September 1992 and June 1995. There were 204 injuries and 20
deaths. 32.4% were outside the minefield demarcation zones, 17.1% in seemingly
demined fields, 13.9% were non-avoidable and 6.9% were mines lost in time. 5
Antibiotic administration first 24hs
Benzyl
Penicillin
9
Benzyl Penicillin with other
Penicillins 5
Benzyl Penicillin with Metronidazole 1
Triplopen with Metronidazole 1
Other Penicillins alone 5
Ampicillin and Metronidazole 1
Tetracyclin/Erythromicine with 1
Metronidazole
The Malvinas War medics who had to amputate limbs
with a Swiss Army penknife - and no anaesthetic .30,34
On May
28, 1982, during the combat of Goose Green, British soldier Dave 'Chopsey' Gray
received a mortar hit that ripped his right leg, tearing left full with
shrapnel. Gray was in a crater flooded with his own blood.
Corporal
Lancer Bill Bentley from Manchester came to assist him and realized that he had
to have his right leg amputated. He took out the only thing he had: his Swiss
Army penknife and, without anesthesia cut
the tissue from which the leg still hung. Then applied a tourniquet on the stump.
Gray was
carried on a stretcher under heavy fire to the aid station where Captain Steven
Hughes paramedic was to assist him. Gray reacted only with the third liter of
blood transfused. Hughes was to attend 34 Paras and twelve Argentines.
Bentley,
who joined the Army in 1970, and served for 17 years, received four medals
including the Military Medal for Courage and the South Atlantic Medal with
Rosette. Bentley subsequently sold his medals which were auctioned at more than
30,000 pounds.
Resusitation-Intravenous fluid
administration.
Cases Average Range
requirement
-----------------------------------------------------------------------------------
Hartmann´s solution (litre) 23 1,5 0.3-3
Blood(Units) 15
3.4
2-7
Polygeline (Haemaccel)500ml 13
1.7 1-3
Considerations
1. Analgesia: All
British patients were administered a dose of Omnopon in the field through a
syringe containing 30 mg of the drug. In those cases in which a delay in the
evacuation was anticipated, two doses were administered. However in two cases
the analgesia was totally ineffective. Jackson et al suggest that
administration of sublingual Buprenorphine would have been better.26
2. Tetanus
immunization: The 23 cases received 0.5 ml IM of antitetanus toxoid in the
resuscitation phase.
3. Evacuation: Under
very risky situations stretchers, a Volvo BV202 vehicle and helicopters were
used.
Note: Omnopon 10 contains 6.72 mg / ml of Morphine HCL, 0.6 mg / ml of
Papaverine HCl and 0.52 mg / ml of Codeine HCl. The Omnopol 20 is equivalent to
10-15 mg of Morphine.
Rehabilitation of British patients
When returning to UK all amputees were referred to Limb Fitting Center. They received their protheses within 24hours. Only 1 of the 12 BKA and 5 of the 8 above the knee had stumps of a conventional accepted length. In some cases the rehabilitation was remarkable. 3 of 12 BKA passed the physical fitness tsts. It is expected that 3 more will do it as well. One of them is employed as a physical training instructor . Four of the BKA group, including those with doublé amputation were discharged. Of the 8 amputees above the knee, the rehabilitation was less striking and onbiously none can run. 6 have been discharged.With regard to upper limb amputees, one was discharged. In this type of amputee the anual test of aptitude in the use of personal weapons is a problem. Of the three patients who continue in service, two approved this test.
When returning to UK all amputees were referred to Limb Fitting Center. They received their protheses within 24hours. Only 1 of the 12 BKA and 5 of the 8 above the knee had stumps of a conventional accepted length. In some cases the rehabilitation was remarkable. 3 of 12 BKA passed the physical fitness tsts. It is expected that 3 more will do it as well. One of them is employed as a physical training instructor . Four of the BKA group, including those with doublé amputation were discharged. Of the 8 amputees above the knee, the rehabilitation was less striking and onbiously none can run. 6 have been discharged.With regard to upper limb amputees, one was discharged. In this type of amputee the anual test of aptitude in the use of personal weapons is a problem. Of the three patients who continue in service, two approved this test.
Compensations
The British Army has
received many criticisms regarding the compensations offered to the personnel.
The British Legion noted in 2007 that a RAF civilian stenographer who had lost
his thumb got 484,000 pounds while a 23-year-old paratrooper Ben Parkinson who
required lifelong support for stepping on an antipersonnel mine received
152,150 pounds. 9
The American program of comrade and
mentor for the amputated war veteran.
The US Veterans Administration Amputee Assistance
System works in conjunction with the Amputee Coalition providing a
successful Amputee Veteran Companions
Program that acts as mentors. Contact is established among veterans who
have suffered the same type (and cause) of amputation and parallels in sex and
age.38
Return to active service
A study conducted by
Kisbaugh (1995) found that only 11 of the 469 (2.3%) of the amputated American
soldiers re-entered the service in 1980. They presented partial amputations of
foot, hand and infrapatelares.18
Nonetheless, and due
to new technologies according to the US Army. At least 167 soldiers with major
amputations have remained in active service since the beginning of the war in
Afghanistan and Iraq.27
The factors that
limit the re-entry of amputees to active service are:
1. Complications in the healing of the
limb.
2. Loss of multiple limbs
3. Phantom Member Syndrome
4. Disturbances that limit the use of
the prosthesis
5. Decrease in functional capacity
6. Traumatic brain injury
7. Delayed psychological adaptation to
amputation
8. Loss of self-confidence to
reintegrate.
Competencies
Approximately 600 US
war veterans participate in Orlando's Wheelchairs
Competition, stimulating them to have healthier and more active lives.44
In 2017 the Chaqueña Selection for
Amputees made a demonstration of discipline in Villa Ángela.
Inability and Disability
Inability in the
workplace is the situation in which a worker is not qualified to perform a job
or any job, depending on the degree of inability. In Argentina, 12.9% of the
population has a permanent difficulty or limitation.12
The most common
inability is the visual one (in Argentina, 264 thousand people suffer it), then
the motor one (110 thousand); the auditory follows (72 thousand) and finally
the cognitive one (55 thousand) .21
A worker can be disabled and have no
inability or vice versa.
Example: A person with hemophilia has a 33%
disability but is perfectly capable of working. A worker with chronic
depression may have a total permanent inability for his or her usual job as a
truck driver but does not have any degree of disability.11
Valuation table for permanent inabilities
43
By amputation of the muscle, between
the hip and the knee, from 70 to 80%.
By amputation of the leg, between the
knee and the neck of the foot, from 55 to 65%
For the total loss of the foot, from 50
to 55%
For the mutilation of a foot with heel
conservation, from 35 to 45%
For the tarsal-metatarsal
disarticulation, from 25 to 30%
In Argentina there is
the National Rehabilitation Service (SNR)
located in Ramsay 2250 (0800-555-3472) that extends the Single Certificate for
Disability. This last is a public document determined by a medical board, which
is granted to any person who requests it and who has a functional, permanent,
transient or prolonged physical, sensory or mental impairment. That in relation
to their age and social environment imply considerable disadvantages for their
adequate family, social or work integration. This certificate allows access a
series of rights and benefits given by laws 22.431 and 24901. The procedure is
free.
Prosthesis
In medicine a prosthesis is an artificial device that replaces a
missing body part, which may be lost through trauma, disease, or congenital
conditions.
Orthesis
An
orthopedic appliance or apparatus used to support, align, prevent, or correct
deformities or to improve function of movable parts of the body.e.g. splints. The orthosis complements but never replaces.
Parts of a prosthesis
- The internal frame, or skeleton, of a prosthetic
limb is called the pylon.
- The socket is the part of the prosthetic
device that connects to the patient's residual limb or limb stump.
- The suspension system keeps the prosthetic
limb attached to the body.
Microprocessors
Microprocessor
is an integrated circuit that contains all the functions of a central
processing unit of a computer.
The C-Leg
is the first prosthesis that has a hydraulic system in the world controlled by
a microchip. With the use of the unique C-Leg technology, a new level of
comfort, safety and mobility has been established for transfemoral amputees.
The Smart
Adaptive has a microchip control. Its sensors analyze speed, slope, stairs
and other parameters.
Amputation levels
1. Hemipelvectomy
2. Hip disarticulation
3. Transfemoral (Above the knee)
4. Transrotuliana
5. Transtibial( BKA)
6. Ankle disarticulation
7. Fingers partial amputation
Leg amputation
1.Transfemoral
(above the knee)
https://es.slideshare.net/Samfrado/prtesis-y-rehabilitacin-de
Socket systems
1. Conical
2. Quadrangular
3. Cat
Cam 16
-amputados
2.Transtibial
(BKA )
Socket systems for BKA
Non
health profesional may skip this section.
Basically
they are: 1) SSWB (Specific Surface
Weight Bearing): a) Type PTB (Patellar
Tendon Bearing), b) Type PTS (Patellar
Tendon Suspension), c) Type KBM (Kondylen
Bettung Munster) and 2) TSWB (Socket with system of discharge and
total contact): a) Lace to Suction and b) Harmony
System (polyurethane liner).
In the PTB, the stump relies mainly on the Subrotulian zone.
The most frequent error observed with the PTB socket is an excessive adjustment in the popliteal area of the stump. 15. The KTB improves the knee lateral stability.
In the PTB, the stump relies mainly on the Subrotulian zone.
The most frequent error observed with the PTB socket is an excessive adjustment in the popliteal area of the stump. 15. The KTB improves the knee lateral stability.
https://www.google.com.ar/search?q=protesis+kbm&tbm=isch&source=iu&ictx=1&fir=NNsOG0enYQsdbM%253A%252CPnE_hcRoTUCJ3M%252C_&usg=__zMDq_Er0a-8AHFBIvKPQ4ydzNKk%3D&sa=X&ved=2ahUKEwjopLKpz8XcAhXMl5AKHYJ5CqgQ9QEwAHoECAUQBA#imgrc=NNsOG0enYQsdbM:
KBM tibial prosthesis with adjustable foot in
equine for underwater activities such as snorkeling.
Nota: In U.S.A. The Hanger Clinic manufactures the ComfortFlex® socket
that accommodates bone, muscles, vessels, tendons and nerve structures to the
residual stump of each patient. It uses a three-dimensional laser system called
Insignia ™ Laser Scanning.
http://www.hangerclinic.com/limb-loss/resources/what-to-expect/Pages/Insignia-Laser-Scanning.aspx
Knee prosthesis
They are made of titanium, steel or aluminum. There
are more than 50 models.
1. Single axis knee: As a hinge.
2. Polycentric knee: It has a more natural twist
3. Intelligent knee: Controlled by microprocessor.
https://es.slideshare.net/Samfrado/prtesis-y-rehabilitacin-de-amputados
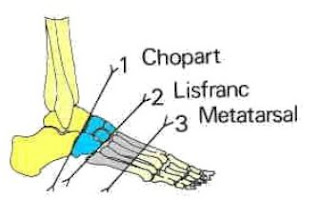
1. Chopart: The foot with an amputation at
the level of the Chopart joint can be difficult to fit, since there is a
remarkable muscular imbalance that tends to place it progressively in equine
and varus.
2. Lisfranc (Tarsometatarsal)
3. Trans-metatarsal
They are made of titanium, steel or aluminum. There
are more than 50 models.
1. Single axis knee: As a hinge.
2. Polycentric knee: It has a more natural twist
3. Intelligent knee: Controlled by microprocessor.
Note: Syme or
Transmaleolar type amputation: Developed in 1842 by James Syme, Scottish
surgeon, this amputation is done leaving the tibia and fibula practically
intact. It consists of a transmaleolar section 0.6 cm above the articular
surface of the tibia and talus. The tissues of the heel are preserved to cover
the stump, which allows the patient to lean directly on it and support its weight,
facilitating walking without prosthesis inside the house. It is indicated in
lesions of the foot with loss of tissues in the vicinity of the tarsometatarsal
joints.
Foot prosthesis:
There are more tan
200 foot prosthesis types.
1. SACH
(Solid
Ankle Cushion Heel): The cushion of the heel absorbs the
impact much like the plantar flexion of a conventional ankle. 42
2. Dynamic
3. Articulated
4.
Energy Vector Optimization EVO. LP Vari-Flex with EVO Ossur.20
(Kindly
submitted by Ally Lou-Nobel China Limited,
Liaobu, Dongguan, Guangdong, China-www.nobel.hk )
Energy saving prostheses
-Hafner,Brian, BS;
Joan E. Sanders, PhD; Joseph M. Czerniecki, MD; John Fergason, CPO Department
of Bioengineering, Department of Rehabilitation Medicine, University of
Washington, Seattle- Transtibial energy-storage-and-return prosthetic devices:
A review of energy concepts and a proposed nomenclature-
Journal
of Rehabilitation Research and Development Vol. 39 No. 1, January/February 2002 Pages 1–11
Flex-Foot Cheetah
http://www.ele.uri.edu/Courses/bme281/F12/LaurenM_2.pdf
Created by 22 years old Van L.Phillips
(who lost his foot in a wáter skiing accident)in collaboaration with an
aerospace company. It´s the only foot prothesis which took part in an Olympic
game. In UK it costs about £ 3700 the pair. 23
Prosthesis for
finger amputation
https://www.google.com.ar/search?q=amputacion+de+dedos+protesis&tbm=isch&tbo=u&source=univ&sa=X&ved=2ahUKEwj0oLTe5t3cAhVEoFMKHSTFACUQ7Al6BAgAEA0&biw=1280&bih=686#imgrc=NJNPZ8hiRW33-M:
See The Evolution of the Robotic Hands -The New York Times Agosto 1,2018:
https://www.nytimes.com/es/interactive/robots-manos-avances/?rref=collection%2Fsectioncollection%2Fnyt-es
The Bionic hand
http://bebionic.com/
Around 600 people in Britain lose upper limbs each year. Current
prosthetic hands work by picking up electrical signals from the stump, but
controlling them requires
practice and concentration. A bionic hand sees an object and reaches for it automatically without
thought.The prosthetic is fitted with a camera which takes a picture of the
object in front of it, assesses its shape and size then triggers an appropriate
grasping movement.The device is ten times faster than current bionic limbs, and uses artificial intelligence to continually improve its detection
and picking-up skills. For the first time in a
century, they had developed an ‘intuitive’ hand that can react without
thinking. The computer isn’t just matching an image, it’s learning to
recognise objects and group them according to the grasp type the hand has to
perform to successfully pick it up. (Sara Knapton-Bionic
hand which see and reaches for objects automatically to be trialled by British
amputees –The Telegraph 3 May 2017).
Scientists in Rome have unveiled the first
bionic hand with a sense of touch that can be worn outside a laboratory. The prosthetic hand has sensors
that detect information about whether an object is soft or hard.These messages
are linked to a computer in a rucksack that converts these signals into a
language the brain will understand.
(Fergus Walsh-Woman receives bionic hand with sense of touch-BBC News 3 January
2018)
It took less than a year since that first hand prosthesis that the
innovators Gino Tubaro and Rodrigo Pérez Weiss printed in 3D for Felipe
Miranda, an eleven-year-old boy. Tubaro won a History Channel award and began working at the Technological Innovation Center. It was set as an example by the
President of the United States. Barack Obama. (Clarin, 3/23/16)
Nicolás Bantar, is one of the ambassadors in Paraná, together with Matías
Agüero, of the NGO AtomicLab, a
non-profit non-governmental organization that prints prostheses of hands and
arms in 3D and gives them free of charge to those who need it.
nodaltec.am /2015/05/jovenes-disenan-una-protesis-de-mano-3d-hiperrealista-y-economica/
Prostheses used in the United Kingdom
The The Limbless Veterans (Blesma ), founded
in 1930, is a British charity that helps all men and women in service and out
of duty who have lost limbs or eyes. They follow the guidelines of prosthesis
dictated by the National Health Service (NHS)8,45
For most primary
amputations below the knee (BKA), they use a PTB (Patellar Tendon Bearing)
socket with an internal lining and some type of suspension with silicones. 10
In the case of foot
amputations, the British usually indicate the Pro-Flex ®XC. Not only is it
useful for walking normally but it is also suitable for those who run or take
long walks.
For transfemoral
amputations, they use an internal lining called Iceross® Seal-In® liners. 10
The NHS provides
prostheses with microprocessors in the cases in which it is indicated.8
Pro-Flex
®XC
Argentine engineer Matías Menghini designed and built a functional
prosthesis of knee and foot flexible prosthesis that will allow, in the near
future, to replace successfully the expensive prosthesis of imported origin
that now dominate the local market .(Diario
Jornada-16 / 3/15) and (Argentina
Investiga 13/4/15)
Osseointegracion.22
Osseointegration,
a process that links the prosthesis directly to the skeleton, can improve the
comfort and mobility of amputees
Commander
Jonathan A. Forsberg, orthopedic oncologist at Walter Reed National Military
Medical Center in Bethesda, Maryland, and a researcher at the Naval Medical
Research Center, treats patients who have suffered recent injuries and those
who have been living with amputations for many years.
"The development of
osseointegration, as a capacity within the Department of Defense, satisfies our
commitment to provide advanced solutions for the entire spectrum of combat
casualty care," said
Forsberg. Although clinical trials have been conducted for osseointegration in
other parts of the world, the Walter Reed clinical trial is the first of its
kind to be conducted in the United States.
The first
patient of the program was former Sergeant Michael Frazier. In May 2011,
Frazier stepped on an improvised explosive device in Trek Nawa, Afghanistan,
losing both legs from the explosion. This patient received another type of
osteointegrated implant from Potter and Forsberg: the Compress® Transdermal
Implant funded by the Department of Defense.
Cost
A person who does not receive a prosthetic within 2
years of amputation has a greater likelihood of social welfare.
For
patients without health insurance, a prosthetic leg typically costs less
than $10,000 for a
basic prosthetic leg up to $70,000.A
computer-assisted prosthetic leg which
controlls muscle movements costs $20,000 or more.
The
C-Leg computerized prosthetic leg by Otto-Bock, for above-the-knee
amputees, can cost as much as $50,000, or up to $70,000 or
more, including the prosthetic foot.
RSL Steeper, creator of the Bebionic artificial hand, has
just announced that the hand will be offered at a price of $11,000 (€9000)
around the world. Amputees control the prosthetic limb using my-oelectric
sensors that read signals on the surface of the skin from residual muscle.
Skinning, poem of Colombian writer Darío Jaramillo 46
Without foot my body keeps loving the
same and my soul goes out to the place that I no longer occupy, outside me: No,
there are no symbols here, the body adapts to the passion and passion to the
body that loses its fragments and continues intact , untouched without
mysteries .
Against death I have the look and the
laughter, I am the owner of my fríend´s hug and
of the dull beat of an anxious heart.
Against death I have pain in a foot
that I no longer have, a pain as real as death itself and a huge desire for
caresses, kisses, to know the proper name of a tree that overlooks me, to
aspire a lost perfume that I pursue , to hear certain songs whose fragments I
remember , to caress my dog, to ring the phone at six in the morning, to follow
this game.
Note: Darío Jaramillo,
author of Memories of a Happy Man,
lost one of his legs as a result of a mine that was not destined for him in
Bogotá in 1982.
Conclusion
Questions are always more important
than answers. There
is no unified registry of the amputations carried out in the Malvinas and many
files are still in the process of being digitized. It would be interesting to
know how many amputees (and other disabilities) exist per province, how they
evolved and if they have sports activities that imply reviewing the type of
prosthesis.
Acknowledgement
-Chenier, Brian-Support Officer
Prosthetics-British Limbless Ex Service
Men´s Association (Blesma)- www.blesma.org. UK
- Clasper, Jon CBE DSc
DPhil DM FRCSEd(Orth), Col L/RAMC,
Emeritus Professor &
Consultant Orthopaedic Surgeon,Military Clinical Director DMG (SE), Visiting
Professor in Bioengineering, Imperial
College London, Clinical Lead, The Royal British Legion Centre for Blast
Injury Studies-UK
-Dra. Diaz Rolon, Gabriela-Chief of
Physiatry -Instituto Nacional de
Servicios Sociales para Jubilados y Pensionados (INSSJP).Argentina.
- Henson, Dave MBE, Department of
Bioengineering, Imperial College London,
South Kensington Campus. UK
-López, Marcela-Librarian-Library of
the Argentine Medical Association. Argentina
-Iglesias, Carlos Col.-Medical
Director of the Argentine Army Central Hospital
Cirujano Dr. Cosme Argerich. H Gral 601.Argentina.
-Lou, Ally-Nobel China Limited- Bohui industrial park, Panlong Road, Yaole 523428, Liaobu, Dongguan,
Guangdong, China.
- Ryan, James Michael Cnel War Veteran OBE, OStJ .
MB, BCh, BAO(NUI), MCh (NUI) (University College Dublin), FRCS(Royal College of Surgeons of England),Hon
FRCEM (CEM) ( Fellow of the College of Emergency Medicine ),DMCC (SoA)(Society of Apothecaries of London).UK
-Tyler, David-National Health Service(NHS). UK
- Szymczak, Marcos- Captain Medicine
Doctor (Ret)War Veteran -Former surgeon
of the Puerto Argentino Military Hospital-
Author of A surgeon in Malvinas published
by the Instituto de Publicaciones Navales.
Argentina
Bibliography
1-Atherton,
Rachel, Robertson, Noelle- Psychological
adjustment to lower limb amputation amongst prosthesis users- Disabil Rehabil. 2006 Oct 15;28(19):1201-9.
2- Bennett Wilson Jr. A. ,
B.S.M.E. - History of Amputation Surgery and Prosthetics-
Chapter 1 - Atlas
of Limb Prosthetics: Surgical, Prosthetic, and Rehabilitation Principles. Digital Resource Foundation for the
Orthotics& Prosthetics Community.
3-Bosmans JC1, Geertzen JH, Post WJ, van der Schans CP, Dijkstra PU. Factors associated
with phantom limb pain: a 31/2-year prospective study- Rehabil. 2010 May;24(5):444-53.
4-Can,
Emine-Prosthesis Support Systems-Fundamentals of Biomedical
Engineering.Universidad Tecnica de Estambul.(Turkey)
5-Castelli, Roberto-Amputaciones
postraumáticas ocasionadas por minas antipersonales. Experiencia en la Guerra
de Yugoslavia. Rev Asoc Argent Ortop
Traumatol –Año 68-pp 303-311.
6-Ceballos, Enrique Mariano Teniente Coronel
Medico, Buroni, Jose Raul Teniente Coronel Medico-La Medicina en la Guerra de
las Malvinas-Circulo Militar,1992.
7- Ceballos, Enrique Mariano Teniente Coronel
Medico, Buroni, Jose Raul Teniente Coronel Medico, Barrera Oro, Ariel Dario-Rev Asoc Arg Ortop y Traumatol. Vol 52
No 3-p269-281.
8-Chenier,
Brian-Support Officer Prosthetics-British
Limbless Ex Service Men´s Association (Blesma)- www.blesma.org (Personal
communication).
9-Chesshyre,Robert-Alive and kicking-The Telegraph-25 Aug 2007.
10- Clasper, Jon CBE DSc
DPhil DM FRCSEd(Orth), Col L/RAMC,
Emeritus Professor &
Consultant Orthopaedic Surgeon,Military Clinical Director DMG (SE), Visiting
Professor in Bioengineering, Imperial College
London, Clinical Lead, The Royal British Legion Centre for Blast Injury
Studies-UK (Personal Commnication)
11-Diferencias entre discapacidad e
incapacidad-Lo Entiendo.
12-El panorama de la discapacidad en
Argentina-INFOBAE-2 de diciembre de 2016.
13- En
Argentina el 48% de las amputaciones son por diabetes-La Nacion, 14 de noviembre de 2005.
14-Espinoza, Maria
Jose, Garcia, Daniela-Niveles de Amputacion en miembros inferiores: Repercusión
en el futuro del paciente. Rev.Med. Clin. Condes - 2014; 25(2) 276-280.
15-Foort,James- The
Patellar-Tendon-Bearing Prosthesis for Below-Knee Amputees, a Review of
Technique and Criteria-Digital Resource
Foundation.
http://oandplibrary.org/al/1965_01_004.asp
16-Gailey, RS et al-The Cat-Cam socket
and quadrilateral socket : a comparison of energy cost during ambulation-Prosthetics and Orthotics International 1993,
17, 95-100
17-Gallagher,
Pamela
PhD &
Malcolm MacLachlan PhD- Psychological Adjustment and Coping in Adults With
Prosthetic Limbs- Behav Med. 1999 Fall;25(3):117-24.
18-Gambell,
Jeff-The Process of Returning to Duty or Not After
Limb Loss-A publication of the Amputee Coalition
of America in partnership with the U.S. Army Amputee Patient Care Program.
19-Groom AFG Maj
FRCS, RAMC, Coull, Brig JT FRCS,
L/RAMC-Army amputees from the Falklands-Review-J R Army Med Corps 1984;130:114-116.
20-Hafner,Brian, BS;
Joan E. Sanders, PhD; Joseph M. Czerniecki, MD; John Fergason, CPO Department
of Bioengineering, Department of Rehabilitation Medicine, University of
Washington, Seattle- Transtibial energy-storage-and-return prosthetic devices:
A review of energy concepts and a proposed nomenclature- Journal of Rehabilitation Research and
Development Vol. 39
No. 1, January/February 2002 Pages 1–11
21-Hay 3,2 millones
de personas con discapacidad en el país-La
voz, 7 de enero de 2012.
22- Health.Mil-The
official website of the Military Health System and the Defense Health Agency.
23- Dave Henson MBE, Department of
Bioengineering, Imperial College London,
South Kensington Campus. UK (Personal
Communication)
24-Horgan, Federico
G., Garay, Rafael, Sangiorgi, Alejandro, Orsi, Hector-Lesiones por el frio.
Experiencia con cámara hiperbarica. Pie de trinchera. Sanidad Naval en
Malvinas. Boletin del Centro Naval-Numero
830-May/Ago 2011.
25-Irvine, Chris-
British
troops in Afghanistan suffer more than 50 amputations-The Telegraph-2 Aug 2009
26-Jackson
DS Maj FRCS, RAMC, Jowitt MD Maj MRCS, FRCP, RAMC, Knight RJ LtCol FFARCS
,RAMC- First and Second Line
Treatment in the Falklands Campaign A Retrospective View- J R Army Med Corps 19R4; 130: 79-83
27-Koebler,
Jason- New Prosthetics Keep Amputee Soldiers on
Active Duty-US News-May 25,2012.
https://www.usnews.com/news/articles/2012/05/25/new-prosthetics-keep-amputee-soldiers-on-active-duty
28-Dr. La O Ramos,
Raidel y Lic. Alfredo D. Baryolo Cardoso- Rehabilitación del
Amputado de Miembro Inferior- Medicina de Rehabilitación Cubana- Camaguey, Cuba, 15 de
septiembre del 2005
29-Mckechnie PS1, John A2. Anxiety and
depression following traumatic limb amputation: a systematic review.- Injury. 2014 Dec;45(12):1859-66.
30-Manchester Evening News-Falklands hero
sells medals-20 jul 2007.
31-Mathews, Jane-Falklands veteran
has leg amputated after stubbing TOE. -Sunday Express--Jul 17, 2014-
32-Melzack, Ronald-Phantom Limbs-Mysteries of the Mind-Scientific American-April 1992.
33-Naschitz JE1, Lenger R.- Why traumatic leg amputees are at increased
risk for cardiovascular diseases-QJM. 2008 Apr;101(4):251-9
34-Nichol, John-Rennell,Tony-The quiet heroes: The Falklands War medics who had to amputate limbs with
a Swiss Army penknife - and no anaesthetic –Mail Online 13 October 2009.
35-Perkins ZB et al- Factors affecting outcome after
traumatic limb amputation-Br J Surg. 2012
Jan;99 Suppl 1:75-86.
36-Pezzin LE
et al- Rehabilitation and the long-term outcomes of
persons with trauma-related amputations. Arch Phys Med Rehabil. 2000 Mar;81(3):292-300.
37- Physical Therapist's Guide to
Below-Knee Amputation-
https://www.moveforwardpt.com/SymptomsConditionsDetail.aspx?cid=c6bc380c-09fc-4dd5-987b-4bbba87e45bc
38-Poorman, Cindy-
VA Amputation Peer Mentorship Program goes
digital-US Department of Veterans Affairs.
39-Rapisarda, Jose Antonio, Setton, Ernesto,
Romero, Roberto Rogelio, Romero, Roberto Hernan, Etchenique, Federico-Primer
simulacro de amputación traumatica de miembro superior de necesidad y rescate
en un escenario inhóspito. Base Marambio. Antartida Argentina-9 de diciembre de
2011-Revista de la Asociacion Medica
Argentina –Vol 125-Numro 2 de 2012.
40-Sahu,
Anamika-Psychological
effects of amputation: A review of studies from India-Industrial Psychiatry Journal-Volume 25-Jan-Jun 2016.
https://www.researchgate.net/publication/311903608_Psychological_effects_of_amputation_A_review_of_studies_from_India
41-Sellegren, Kim R.-An
early history of lower limbs amputations and prostheses-The Iowa Orthopaedic Journal- Iowa Orthop J. 1982; 2: 13–27.
Orthopedics & Prosthetics Appliance Journal-June-August 1957.
http://www.oandplibrary.org/op/pdf/1957_02_023.pdf
43-Tabla de Valuacion de Incapacidades Permanentes
https://sjf.scjn.gob.mx/sjfsist/Anexos/0041002903993.pdf
44-Tostenrude,Dave-National
Veterans Wheelchair Games-
More than 3,000 volunteers needed for the 38th National Veterans Wheelchair
Games-US Department of Veterans Affairs.
https://www.blogs.va.gov/VAntage/44472/3000-volunteers-needed-38th-national-veterans-wheelchair-games/
45-Tyler, David-David Tyler -National Health Service(NHS). Reino
Unido.(Comunicación personal)
46-Una mirada personal sobre los
grandes temas cotidianos:Perder una pierna no es perder la pasión por la vida. Clarin Junio 16, 2012.